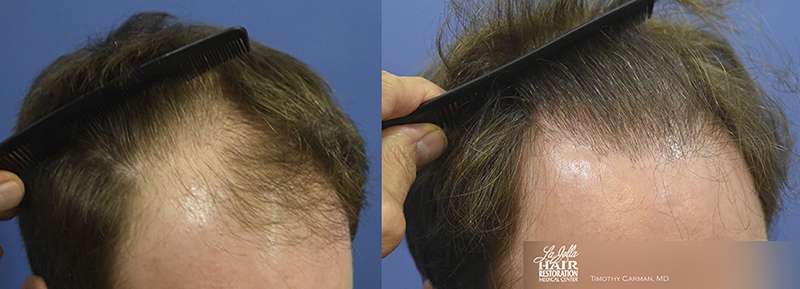
FUT Hair Transplant Case Study – 1849 Grafts at 9 Month Follow Up
History: This patient is a pleasant 29 year old male who experienced thinning of his fronto-temporal hairline since the age of 20. He is generally very healthy, with no medical history or previous surgeries.
He has become progressively more and more pre-occupied with his hair loss as it has affected his self-esteem, limiting his social activities. The frontal thinning becomes especially apparent after exercise, as the thinning becomes more noticeable when his hair is wet.
His family history is significant for fronto-temporal thinning in a similar pattern in his father, 64, that has progressed about midway into his midscalp, with no apparent crown involvement.
The patient has decided that he does not want to utilize finasteride as a medical therapy now or in the foreseeable future.
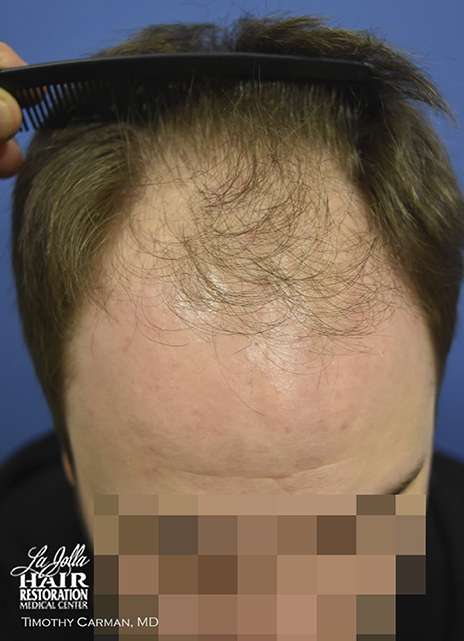
Top view prior to hair transplant surgery.

Left front view prior to FUT hair transplant.
Physical Exam: The patient has brownish-blonde (“dirty-blonde”) colored hair with strands of medium thickness that has a mild curl at lengths greater than 4- 5 cm. He presented with total loss of the fronto-temporal hairline and frontal forelock area, and significant loss of density (due to miniaturization) in the anterior midscalp area. His donor area showed a density of 80-90 follicular units per square cm, which is considered average. Based on the anticipation of future losses, a “conservative” hair line was designed. (A “conservative” hairline is one which has some bilateral recession built into it; it is a design that is “forward-looking”, in that it will age with the patient and conserve grafts for use later on down the road for other areas that may thin.) We planned to rebuild the frontal forelock area and the anterior midscalp as well. Our plan was centered around 1800 FU grafts.
Procedure: On the morning of the procedure, our surgical plan was revisited, and the hairline was drawn according to the surgical design which was discussed with the surgeon in detail during the initial consult. The safe donor area was then identified, and the appropriate length and height of the strip determined based on the number of follicular units (which will become our “Grafts”) decided upon previously.
In most all cases, the hair is preferably left at a length of an inch or more, as the hair will completely cover the area where the donor was removed following excision. The strip is typically about one to one and a half centimeters in height, (about1/2 inch) and it’s length dependant on the number of grafts needed. In this case the length was 15 centimeters (about six inches). The patient is sitting upright in the surgical chair, and small amounts of lidocaine are instilled in a circle around the patients head. This takes about two minutes, and is the “uncomfortable” part of the procedure due to the slight burning of the medication.
Once completed, the entire donor area as well as the area to be transplanted is completely numb. The donor was then removed, and a plastic surgery style closure was utilized to create a very minimal appearance upon healing. The donor site is then placed in the care of the surgical team that will create the 1, 2 and 3 hair grafts from the naturally occurring 1, 2 and 3 hair follicular units, by dissecting them under direct visualization utilizing microscopes. During this time, the patient was placed in the reclining position to enjoy a movie, music, or simply snooze. While the grafts are being prepared, the recipient sites were created, by hand, by the surgeon. This step is essentially sculpting, and an eye for artistic detail is critical. Angulation of the sites, dispersal of the various types of grafts, and varying density are all elements the surgeon addresses in order to create a natural, organic pattern which will be undetectable as man made. In our practice, all blades utilized for this step are created on the spot to specifically fit the individual tissue characteristics of the specific patient on the day of surgery.
Creation of sites should only be performed by the surgeon. Following this, the grafts were placed by three members of the surgical team, in order to decrease the “out-of the-body” time of the grafts. The procedure took about 8 ½ hours total.
Results
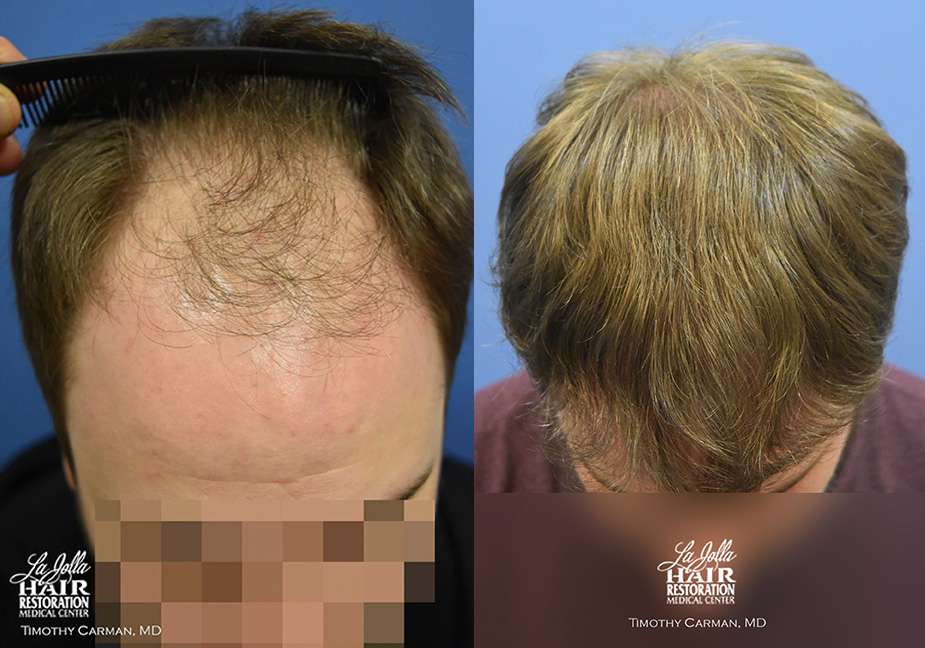
Before and 9 months after 1849 grafts transplanted. Top view.
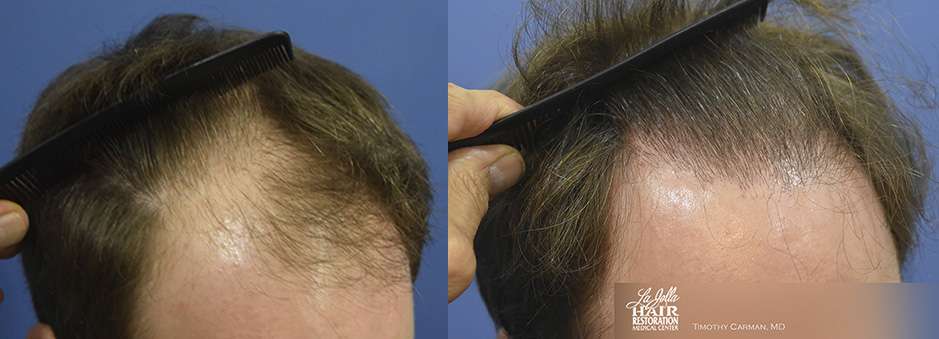
Before and after 1849 grafts – post-op 9 months
Results: A total of 1829 FU grafts were obtained as follows; 743 one hair grafts (utilized as the leading edge of the hairline); 1086 two and three hair grafts (to add density behind the hairline and in the midscalp area). The result shown is at the 9 month mark. At this stage there is typically about 80% growth seen, so there will be some additional subtle filling in over the next 3- 4 months.
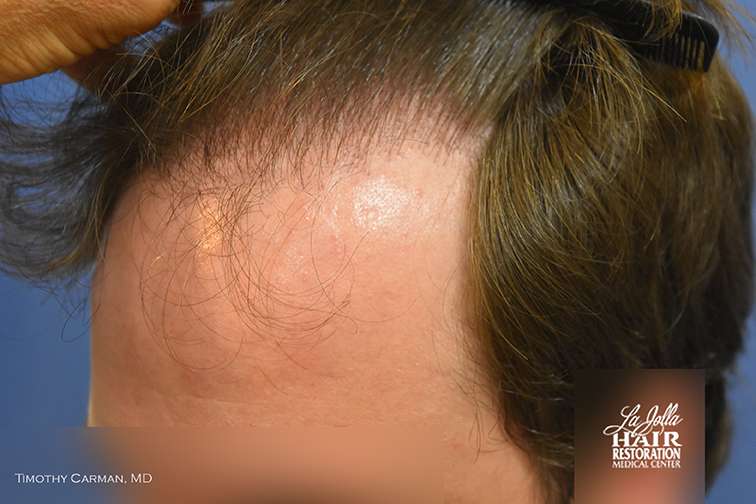
Right side view post-op 9 months.
Discussion: This case illustrates several points. Most importantly, the planning which needs to go into the surgical design. There is a limit to the amount of donor all patients have over their lifetime, and in a young patient it is critical they understand how this fact directly affects the artwork that can be accomplished according to the surgical design.
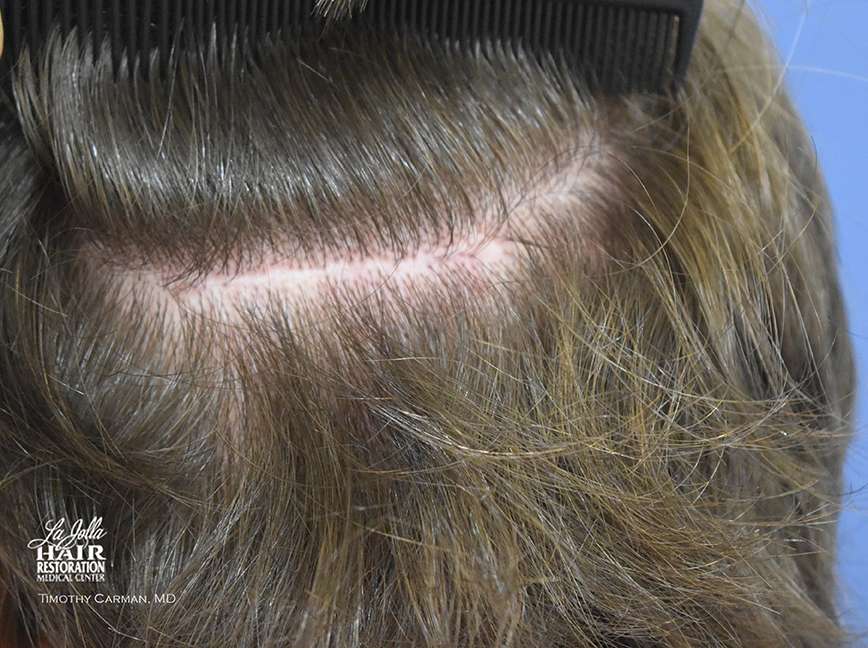
Donor scar is virtually invisible without close inspection.
This is why in our practice philosophy it is critical that the surgeon perform the surgical consult in detail well in advance of the procedure, as the surgical design is the blueprint upon which the current and future procedures will be built. This is also in line with standard of care practices in Plastic as well as General Surgery. The case also illustrates the typical close cooperation between the surgeon and surgical assistants; experience and ethical standards are the cornerstone of a successful practice, and this, in our opinion, can only be found most consistently in practices dedicated solely to the practice of treating hairloss via transplantation and other adjunctive medical and surgical therapies.
As with all hair transplant procedures, this case also illustrates the artistic nature of the process. To me, as a surgeon, the creation of the sites is an absolute pleasure, and as an artist there is no detail too small, especially when it comes to making custom-sized surgical blades specific for each patient. This is often overlooked in many practices, as utilizing commercially made blades which are available are the norm. I borrowed this concept from my habits as an oil painter. I create my own brushes for detailed work- and have done so for decades. It allows me to address the specific needs of the project I am working on at that time.
In hair transplant, although there are generalities across all patients that provide the “basics” of the hair transplant procedure (observing these makes for consistent results), there are details specific to each patient that makes each case unique. It is the recognition of those details and addressing them that elevates the procedure from one of rote repetition to one of true artwork.
This patient, through a successful transplant procedure, has regained his confidence and self-esteem as a result of the surgical team’s dedicated and conscientious work. There is no greater reward than being able to contribute to an improvement in the quality of life of our patients, and this patient, as with all our patients, illustrates this last point as very well.